Disorders of the Nervous Systems
Please visit our Neurology or Neuropathy page for more details.
Nerves, together with the spinal cord and brain, control so many diverse functions that there are over 600 documented nervous diseases. They cover areas such as movement, speech, memory, and mood.
Below are some of the areas we focus on at our Phoenix Neurology office.
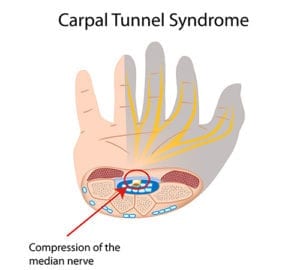
Carpal Tunnel Syndrome (CTS)
Carpal Tunnel Syndrome (CTS): Sometimes known as a trapped nerve, Carpal Tunnel Syndrome (CTS) is often caused by direct pressure on the median nerve in the wrist. Symptoms include pain, numbness, and a “pins and needles” feeling similar to a limb falling asleep. The condition usually results from a combination of environmental and genetic factors, such as diabetes, obesity, pregnancy, hypothyroidism, or heavy manual work that may involve vibrating tools. The main symptom of CTS is intermittent numbness of the thumb, index, and ring fingers. Often the symptoms are felt more at night, since many people sleep with their wrists flexed or bent. This numbness can be so intense that it wakes one from sleep. Untreated CTS can eventually lead to permanent nerve damage, constant numbness, and weakness or even atrophy of the muscles in the palm and at the base of the thumb.
CIPD
Chronic Inflammatory Demyelinating Polyneuropathy (CIPD): also known as chronic relapsing polyneuropathy (CRP) or chronic inflammatory demyelinating polyradiculoneuropathy. It is an acquired immune-mediated inflammatory disorder. In simpler terms, this means that the immune cells in the body, which normally fight infection, are incorrectly attacking nerves in the body. The nerves produce responses that include numbness, tingling, muscle weakness, fatigue, and pain. CIPD is closely related to Guillan-Barré Syndrome and is considered to be the chronic, or long-term, equivalent to that acute disease.
Guillain-Barré syndrome (GBS) is a disorder in which the body’s immune system attacks part of the peripheral nervous system. The first symptoms of this disorder include varying degrees of weakness or tingling sensations in the legs.
Guillain-Barré Syndrome is a rare syndrome is not contagious but can affect anybody – any age, gender, ethnicity. Usually Guillain-Barré occurs a few days or weeks after the patient has had symptoms of a respiratory or gastrointestinal viral infection. Occasionally surgery will trigger the syndrome. After the first clinical manifestations of the disease, the symptoms can progress over the course of hours, days, or weeks. Most people reach the stage of greatest weakness within the first 2 weeks after symptoms appear, and by the third week of the illness 90 percent of all patients are at their weakest.
There is no known cure for Guillain-Barré syndrome. Therapies that lessen the severity of the illness and accelerate the recovery are plasma exchange (also called plasmapheresis) and high-dose immunoglobulin therapy. Patients usually reach the point of greatest weakness or paralysis days or weeks after the first symptoms occur. Symptoms then stabilize at this level for a period of days, weeks, or, sometimes, months. The recovery period may be as little as a few weeks or as long as 3 years. About 30 percent of those with Guillain-Barré still have a residual weakness after 3 years.
External Resource: The National Institute of Neurological Disorders and Stroke
Fasciculation
Fasciculation: also known as muscle twitch, is a small, local, involuntary muscle contraction and relaxation which may be visible under the skin. Deeper areas of this condition can be detected by electromyography (EMG) testing, although it can happen in any skeletal muscle of the body. Fasciculations occur due to spontaneous depolarization, or an electrical activation of the lower motor neurons, which then signal the skeletal muscle fibers of a single motor unit to contract at the same time. An example of normal spontaneous depolarization is the contractions of the cardiac muscle, which cause the heart to beat. Usually, the fasciculations stop once the involved muscles are intentionally moved (a person feels a muscle in his leg twitch, so he shakes his leg up and down), but they may return once the muscle is at rest again.
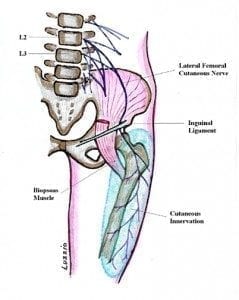
Meralgia Paresthetica
Meralgia Paresthetica: is a numbness, tingling, or pain in the outer thigh that is not caused by an injury to the tissue, but by a compression of the lateral femoral cutaneous nerve, which extends from the thigh to the spinal column. Obesity, pregnancy, or any situation that causes increased pressure on this nerve (such as wearing a heavy tool belt) are often factors in this condition.
Nerve Entrapment
Nerve Entrapment: also known as nerve compression syndrome, compression neuropathy, or entrapment neuropathy, is a medical condition caused by direct pressure on a single nerve. In layman’s terms, it might be referred to as a trapped nerve, although this expression is used for a variety of conditions (e.g. a herniated disc). Symptoms of nerve entrapment include pain, tingling, numbness, and muscle weakness in a particular part of the body, depending upon the nerve affected.
Numbness
Numbness and Tingling: abnormal sensations that can occur anywhere in the body but are often felt in the fingers, hands, feet, arms, or legs. Often these sensations indicate another possible condition, such as the following:
- Carpal tunnel syndrome
- Diabetes
- Hypothyroidism (underactive thyroid)
- Migraines
- Multiple sclerosis
- Raynaud’s phenomenon
- Seizures
- Stroke and Transient Ischemic Attack (TIA)
Peripheral Neuropathy
Peripheral Neuropathy: damage or disease affecting nerves, which may affect sensation, movement, gland or organ function, and other aspects of health, depending upon the type of nerve affected. Diseases such as diabetes or leprosy, vitamin deficiency, or medication (e.g. chemotherapy), traumatic injury, excessive alcohol consumption, immune system disease, or infection are often causes. It may also be present from birth. Peripheral Neuropathy may be chronic, where it starts slowly and progresses slowly, or it may be acute, with a sudden onset and rapid progress. Acute neuropathies demand urgent diagnosis. Peripheral Neuropathy may involve motor nerves (that control muscles), sensory nerves, or automatic nerves (that control heart rate, body temperature, and breathing.) The effects of this condition depend upon the nerve involved. Some examples include the following:
- Motor: impaired balance or coordination, muscle weakness
- Sensory: numbness to touch or vibration; reduced sensitivity to temperature and pain; reduced ability to sense the body’s position, resulting in poor coordination and balance.
- Automatic: poor bladder control, reduced ability to sweat normally, abnormal blood pressure or heart rate.
RSD / CRPS
Complex regional pain syndrome (CRPS): formerly known as reflex sympathetic dystrophy, is an amplified musculoskeletal pain syndrome (AMPS). It is a chronic, systemic disease that is characterized by severe pain, swelling, and changes in the skin. CRPS initially affects a single limb and often spreads throughout the body, worsening over time. In addition to the amplified pain signals, it can cause swelling of the central nervous system, blood flow problems, and sensitivity to things that normally would not cause pain (such as a light touch). Over time, it can also cause changes to the brain as it adapts to the constant pain signals and eventually may lead to impairment and disability in multiple parts of the body. CRPS is unfortunately one of the most painful long-term conditions a person can have. In addition to the recognized effects, there are sometimes additional internal complications to the gastrointestinal, cardiac, respiratory, endocrine, and urological systems. CRPS is sometimes confused with fibromyalgia and multiple sclerosis, as the conditions have similar symptoms.
External Resource: International Research Foundation for RSD / CRPS